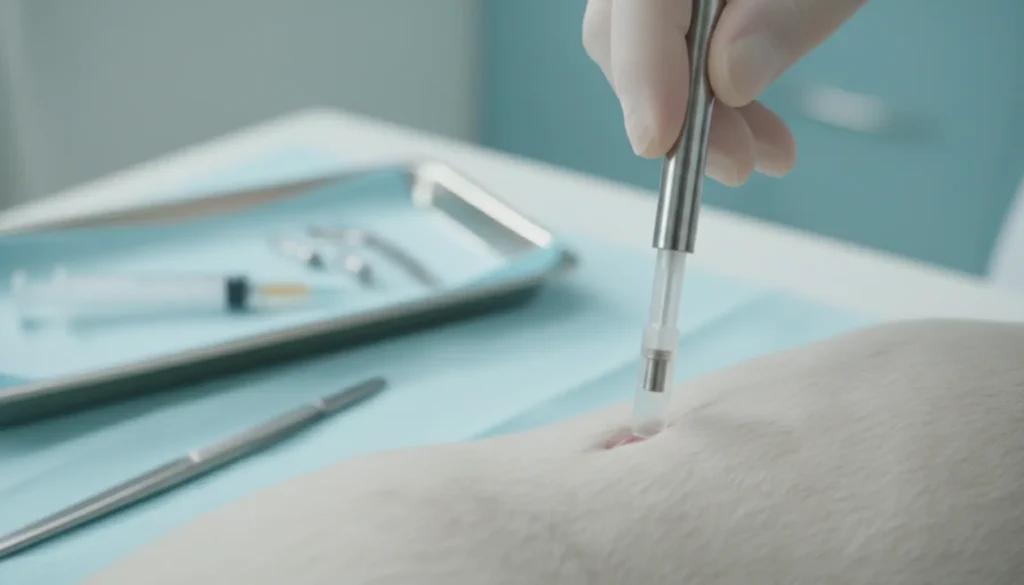
Chemical castration of dogs is an effective way to control fertility without permanent surgical intervention. With this method, caregivers can postpone the decision for permanent castration or choose not to proceed with it at all. Modern implants such as Suprelorin offer temporary sterilization, minimizing risk and providing comfort for both dogs and their owners.
Table of Contents
- What is chemical castration?
- Comparison of castration methods: chemical vs surgical
- How does Suprelorin work on dogs?
- Benefits of choosing chemical castration
- Drawbacks of chemical castration: What to consider?
- Is chemical castration suitable for your dog?
What is chemical castration?
Chemical castration is a modern, pharmacological method for temporarily disabling fertility in dogs by inhibiting the production or activity of sex hormones without permanent surgical intervention. In practice, this means the dog becomes unable to reproduce, and its hormonal balance changes—similarly to traditional surgical castration, but in a reversible way. The most commonly used form of chemical castration in male dogs is hormonal implants placed subcutaneously, which gradually release an active substance (e.g., a GnRH analogue like deslorelin). Their mechanism is to “block” the hypothalamus–pituitary–testes axis, which leads to reduced testosterone levels and inhibits sperm production. From the outside, the procedure is quite simple: in a veterinary clinic, the doctor places a small implant under the dog’s skin, usually at the scruff or between the shoulder blades—resembling a regular vaccination, without anesthesia, cutting, or sutures. After implantation, there’s a transition period in which hormone levels may fluctuate slightly, followed by a stable drop in testosterone, resulting in suppressed sexual drive and loss of fertility.
Unlike surgical castration, where the testes are permanently removed, chemical castration does not cause irreversible anatomical changes—the testes remain in place, although they usually shrink over time due to suppressed activity. The key feature of this method is temporality: the implant works for a fixed period (e.g., about 6 or 12 months, depending on the product and the dog’s individual response), after which its effect gradually fades. When the active substance stops being released, the hormonal axis is “unlocked”, testosterone levels normalize, and fertility and typical male behaviors return. This gives the owner a unique opportunity to test how the dog will function “post-castration” before making a final surgical decision or continuing with further chemical castration implants. It’s important to stress that chemical castration is not the same as short-term hormonal injections known years ago—modern implants provide more stable, predictable, and safer effects, and their reversibility is well documented in veterinary literature. This method is primarily intended for males and is used both for conscious reproduction control (e.g., in breeding dogs where future reproduction is planned) and for modifying behaviors related to high testosterone, such as intense urine marking, escaping to females in heat, or increased rivalry with other males. Although the fundamental assumption of chemical castration—temporarily limiting fertility via hormonal manipulation—is relatively straightforward, the exact details, dosage, duration, and potential side effects should always be discussed individually with a veterinarian, as dogs may respond differently, and the decision should take into account the animal’s age, health, weight, and breeding plans.
Comparison of castration methods: chemical vs surgical
Chemical and surgical castration both lead to similar functional outcomes—limiting fertility and often modifying behaviors related to sex hormones—but the manner, duration, invasiveness, and possible side effects differ fundamentally. Surgical castration (orchidectomy) involves the permanent removal of the testes under general anesthesia, irreversibly stopping testosterone and sperm production. It’s a one-time procedure performed in veterinary offices and clinics, providing a predictable, permanent result and significantly reducing the risk of certain diseases, such as testicular tumors or prostate issues later in life. Chemical castration works differently: the implant releases an active substance that “switches off” the fertility-related hormone axis for a defined period, without physically removing the organs. This means it is reversible; the effect wears off naturally after several months or a year. Differences arise at the preparation stage—surgical castration requires pre-anesthesia qualification tests (including blood tests, often ECG in older dogs), proper preoperative preparation, and post-op care, wound protection, use of an Elizabethan collar, and often limiting activity for at least a couple of weeks. Chemical castration is usually a quick procedure performed “at the table”, no general anesthesia required—in most cases, a brief restraint and subcutaneous implant insertion is sufficient, and the dog returns to normal activity almost immediately after the visit.
An important comparison element is reversibility and decision flexibility. Surgery is final—once removed, the testes cannot be restored; owners who change their minds or want offspring later no longer have that option. Chemical castration is a “trial period”: it allows the owner to see how the dog responds to lower testosterone, behavioral changes, appetite, or body mass, before making an irreversible decision. This is particularly valuable for young dogs showing early behavioral issues such as escaping to females, excessive marking, or rivalry aggression with other males—the implant provides a chance to assess if “hormonal calming” genuinely helps, without committing to permanent castration if results are unsatisfactory. On the other hand, repeated chemical procedures (every 6–12 months or as the vet advises) can become more costly long-term than a one-time surgery, especially for young dogs who would need implants for many years. It’s also worth noting differences in action dynamics—after surgical castration, the testosterone drop is fairly quick and permanent, but with chemical implants there’s an initial, short-lived “calming phase;” behavioral and fertility changes may only emerge after several weeks and are gradual, with hormone levels rising again as the implant wears off—which may mean a return of previous problems. Health-wise, each solution has pros and cons—surgery reduces the risk of testicular cancer to zero and notably diminishes various prostate disorders, but comes with a (usually small) risk of surgical complications, wound infections, or unfavorable metabolic changes such as weight gain. Chemical castration avoids surgical and anesthesia risks and is generally more accepted by owners afraid of anesthesia, but can cause other side effects, such as temporary behavioral changes, fluctuations in body mass, or changes in coat appearance; the dog’s current health during implant use is not as well documented as with surgically castrated dogs. There are psychological aspects as well—many owners find comfort knowing that fertility will return if needed, easing them into the idea of castration, while others prefer “one cut and it’s done” to avoid revisiting the issue every few months. Ultimately, choosing the best method requires a discussion with a veterinarian who can compare options in the context of the dog’s age, health, breed, prior behavioral issues, and breeding plans.
How does Suprelorin work on dogs?
Suprelorin is an implant containing deslorelin, a synthetic analogue of the hormone GnRH (gonadoliberin), which is naturally produced in the hypothalamus and regulates testicular function via the pituitary gland. Suprelorin’s mechanism is based on so-called “down-regulation” of receptors: after single implantation the preparation releases small regular doses of the active substance into the dog’s bloodstream, which initially briefly stimulates and then suppresses the hypothalamus–pituitary–gonadal axis. In the initial phase, which usually lasts a few days up to 2–3 weeks, there can be a temporary increase in testosterone, as the pituitary responds to the sudden “dose” of GnRH analogue by increasing secretion of LH and FSH—the hormones that stimulate the testes. During this time, some dogs may show intensified sexual behaviors, such as heightened marking, increased interest in females, or occasional attempts to mount, so owners should be prepared and, if needed, limit contact with unspayed females.
After this initial stimulation period, the crucial stage follows: GnRH receptors in the pituitary become “fatigued” by constant stimulation and shut down, leading to a sudden drop in LH and FSH secretion. Without these hormones, the testes stop receiving signals to produce testosterone and sperm, gradually lowering hormone levels in the blood and suppressing fertility. In practice, about 4–6 weeks after implantation, most dogs achieve the state of effective “functional castration”: they lose fertilization ability, and behaviors linked to high testosterone (e.g., persistent chasing of females, intense marking, some aggressive rival behaviors) weaken. The implant is placed subcutaneously, usually around the shoulder blades or in the neck, using a special applicator similar to a thicker needle. The procedure takes a few minutes and usually does not require general anesthesia, with discomfort similar to vaccination, although sensitive dogs may be offered local numbing or mild sedation. Suprelorin comes in two main doses—a 4.7 mg implant, working for at least 6 months, and a 9.4 mg version with effects for at least 12 months, though actual duration may vary with individual sensitivity, body weight, age, and the dog’s metabolism. While the implant does its work, the testes generally contract and become softer to the touch, which is typical for decreased testosterone, but after it “wears off”, both their size and function usually return to near-baseline, alongside the dog’s reproductive ability. This return of fertility can take from several weeks to a few months, so owners wishing to breed later should discuss their plans and appropriate timeframes with their vet. Note that each dog may react differently to Suprelorin: in some, the behavioral effect (calming, less interest in females, reduced sexual motivation) is pronounced and quick, in others changes are milder or take longer—particularly if problem behaviors are primarily learned rather than hormonal. For this reason, it’s often recommended to combine chemical castration with behavioral work and training, making best use of the period of lower testosterone to consolidate desirable habits. The veterinarian may also recommend monitoring body weight, skin, coat, and general activity since hormonal changes can influence metabolism and appetite—though typically these effects are milder and more manageable than after surgical castration.
Benefits of choosing chemical castration
Chemical castration brings multiple benefits for both the dog and its owner, with the primary advantage being the reversibility. Unlike in surgical castration, where removed testes cannot be restored, a hormonal implant enables a “temporary switch-off” of reproductive function without permanent tissue damage. After the implant’s effect fades, the hormone balance gradually returns to baseline, and the dog may regain fertility—crucial for breeders or those not yet sure of making a final decision. Thus, chemical castration is useful as a “trial period”—the owner can observe how the dog behaves with lower testosterone: whether his attitude, aggression, interest in females, or escape behavior changes. If results are satisfactory, the implant can be renewed or the owner can choose traditional surgery; if not, the dog’s physiology will, over time, return to previous status. This flexibility and ability to change one’s mind provide major emotional support, especially for those afraid of irreversibility.
Another benefit is minimal invasiveness. Implantation uses an applicator similar to a thicker needle, takes just a few minutes, and does not generally require general anesthesia or hospitalization. No surgical cut means no scars, sutures, licking issues, or risk of infection, hematoma, or wound splitting. This is vital for senior dogs or those with heart, kidney, or liver diseases, for whom anesthesia might be unadvisable or risky. For fearful dogs or those struggling with clinic visits, the process is also less stressful as it avoids typical surgical cues like hospital stays, IVs, or Elizabethan collars.
Behavioral benefits are also significant, improving life for both the pet and household. Lower testosterone through the implant usually lessens sexual drive-related behaviors: persistent sniffing for females, howling, restlessness, urine marking at home, or escape attempts during nearby heats. Many dogs also become less excitable and impulsive, making obedience training and behavioral work easier. In some cases, male-male aggression reduces, though always remember aggression has complex origins—castration, chemical or surgical, is not a “magic cure” but rather one tool alongside training and behavior therapy. Chemical castration helps clarify which problems have a hormonal basis and which stem from other factors (fear, past trauma, poor socialization). If aggression or hyperactivity decrease post-implant, the owner and specialist gain a critical hint that permanent surgical castration could make sense. Health-wise, the method allows for temporary reproduction control, avoiding unplanned litters and lowering the risk of accidental breeding, while leaving the door open for future planned mating. Because the solution is reversible, it works as a temporary fix: for example, when a young male and an unspayed female live together and the owner wants to delay reproduction, or if general anesthesia must be postponed due to a chronic illness. Temporal flexibility is also key: various implant durations are available on the market, letting owners choose effects lasting from several to over a dozen months. For young dogs, a single implant can provide stability during the stormiest puberty phase, allowing for an assessment of behavior with reduced hormones, without taking a final step. Owners may appreciate that the testes remain, even though they contract, so the dog’s appearance doesn’t radically change as it would after surgery—important for show breeds or people uncomfortable with organ removal. All these aspects make chemical castration a modern, flexible tool for managing behavior and fertility, letting caregivers combine care for health and welfare with personal comfort and peace of mind.
Drawbacks of chemical castration: What to consider?
Despite its many advantages, chemical castration has drawbacks and limitations to consider before choosing it for your dog. One primary downside is its temporary nature—to maintain the “switch-off” of fertility and low testosterone, regular repeat procedures are necessary every few or several months. This means ongoing vet visits, more doses, and recurring costs that may, over time, surpass the cost of a single surgical castration. Furthermore, the duration of the implant’s effects is not always perfectly predictable—some dogs may lose effect earlier or maintain it longer than declared by the manufacturer, necessitating careful observation and, if needed, monitoring tests. Be aware too of the so-called initial “hormonal flare”: for the first days or weeks post-implant, testosterone may temporarily increase, intensifying sexual behaviors—marking, chasing females in heat, or conflicts with other males. Owners seeking immediate calming may find this period frustrating, requiring extra safeguards and supervision.
Another aspect is that while chemical castration is relatively safe, it still interferes with the hormonal system and can cause side effects in some dogs. These may include local irritation, swelling or pain at the implant site, periods of apathy or, alternatively, hyperactivity, appetite changes, weight gain, or coat changes (dullness, thinning). There are occasional cases where the implant fails to work as expected—testosterone doesn’t fall sufficiently, and fertility and sexual behaviors aren’t fully suppressed. This “resistance” means another solution, typically surgical, must be considered, lengthening the process. Lack of immediate reversibility can be troublesome too—even though the method is theoretically reversible, once implanted, you can’t “turn it off on demand”, and the body needs time after expiration to restore normal hormonal function.
Chemical castration doesn’t provide the full health protection that surgical castration can. Since the testes remain, the risk of testicular tumors or torsion isn’t eliminated, and in some cases, effects on prostate disease are less predictable. The long-term impact of implants over many years isn’t as well researched as the long-used surgical method, which may cause some reserve among owners and vets. Consider behavioral effects too—even though testosterone reduction lessens rivalry, marking, or wandering for many males, not all behavioral problems are hormonal. Thus, even with chemical castration, a dog may remain fearful, hyperactive or aggressive due to socialization issues, trauma, or upbringing errors, so the expected “miraculous improvement” may not come. Owners may also be disappointed to find high energy in working or herding breeds remains, as it’s tied to genetics and selective breeding.
There are practical issues too: the implant, although small, is a foreign body in subcutaneous tissue. There is minimal risk it may shift, fragment, or become untraceable if early removal is needed. Some dogs may have temporary tenderness at the site and may irritate it by licking. Finally, chemical castration may be harder to access at smaller clinics, particularly outside larger cities, and more expensive over years, making it a significant financial constraint for some. All these factors mean the decision about chemical castration should take into account not just comfort and reversibility, but also practical, financial, health, and behavioral realities for every individual dog.
Is chemical castration suitable for your dog?
Assessing whether chemical castration is the right choice for your dog requires looking beyond just caregiver convenience. Key factors are age, health, activity level, temperament, breeding plans, and living environment. The best candidates are usually male dogs where surgical castration is being considered, but the owner isn’t ready to finalize the decision—often young dogs whose reactions to lowered testosterone on behavior, appetite, or physique are still unknown. Hormonal implants are a good option for dogs where general anesthesia would be risky for medical reasons (heart disease, clotting issues, old age, or complications from previous anesthesia)—here chemical castration can be a safer alternative. It is also worth considering when a male lives with a female who is not planned to be spayed soon—the implant can prevent accidental mating and alleviate frustrating behaviors in males during her heat. By contrast, breeding-valuable dogs, or breeds in which delaying/restricting testosterone might affect musculoskeletal development (e.g., large and giant breeds), require extra caution and personalized plans—the veterinarian may advise waiting for castration until growth is complete or implanting only after full physical maturity. Temperament matters too: fearful or overly sensitive dogs may experience heightened insecurity when testosterone drops, needing closer observation and cooperation with a behaviorist. Chemical castration is especially helpful for dogs showing strongly hormone-linked behaviors—persistent marking at home, excessive interest in females, escapes in search for a mate, increased agitation during nearby heats—as it allows you to test whether these issues will lessen at lower testosterone. If there is clear improvement, the caregiver may then confidently consider surgical castration, knowing what to expect.
Your situation as caretaker—emotional, financial, organizational—is also crucial. The implant must be renewed, typically every 6–12 months, sometimes earlier, and requires regular appointments and budgeting, as repeated chemical castration may end up more expensive than a single surgical procedure. Owners who value reversibility and may wish to regain their dog’s fertility (e.g., are undecided about breeding) will particularly benefit from the flexibility of this method—after the implant wears off the dog gradually regains full reproductive capacity, but timing is individual and may vary from several weeks to many months. Be honest about your own feelings towards surgery—many people dislike organ removal for emotional or ideological reasons, but still need to control reproduction and behavior; in such cases, chemical castration is a compromise, lowering stress and avoiding immediate irreversibility. By contrast, if you live somewhere where implants are hard to access, travel to the clinic is a challenge, or frequent visits are very stressful for your dog, a one-time surgical solution may be more practical. Also remember not all behavioral problems are hormonal—fear aggression, bonding disorders, frustration, or lack of stimulation require training solutions, not just hormone reduction, so before deciding, consult both a veterinarian and, ideally, an experienced behaviorist to assess whether any form of castration will genuinely help your dog. Medically, take into account chronic illnesses, current medications, weight, breed tendencies (e.g., obesity, endocrine disease, cancer), and how a drop in testosterone might influence mood and metabolism; some dogs may gain weight, become less active, or develop coat changes, requiring dietary and exercise adjustments. A calm, in-depth talk with your vet—presenting your concerns, expectations, and describing your dog’s medical history—lays the foundation; from here, the specialist can advise whether in your specific case chemical castration will be a temporary solution, a long-term strategy, or if it’s simply not the best choice for your pet.
Summary
Chemical castration is a modern, reversible sterilization method that offers many advantages, including avoiding surgery and being less invasive. Compared to traditional surgical castration, Suprelorin implants provide effective fertility suppression in dogs while reducing risks related to surgical complications. However, choosing the right method should always be thought through and discussed with your veterinarian, taking into account your pet’s health and needs. Chemical castration can be an excellent solution for owners seeking less invasive options.